Whether you’re a Surgeon, Emergency Medicine Physician, Physician Assistant, Nurse Practitioner, Resident, or other Medical Professional working in a facility that requires certification in Advanced Trauma Life Support (ATLS), this course will help prepare you to take the ATLS Certification or Recertification exam with confidence.
Yes, DEFINITELY good match for me. The short quick lectures done by a very experienced speaker are perfect for this course. Its obvious this person has been there and taken care of many trauma patients and can mention the pearls and pitfalls that everyone needs to know.
Michael Heard
[Udemy Review]

Kaylene WeirCox, MD, FACS
Dr. Kaylene WeirCox is board-certified in both general surgery and lifestyle medicine. Her desire to do the most good for people has led her out of the active operating room and into the lifestyle center to help people get to the root causes of their health challenges and make changes before surgical intervention is necessary.
Dr. WeirCox is also the creator of the Ultimate ATLS 10 Prep course that assist doctors, nurses, and other medical professionals prepare for the Advanced Trauma Life Support certification test. This course has been taken by medical professionals in more than 30 countries.
Dr. WeirCox currently services as the Medical Director for Uchee Pines Institute’s Lifestyle Center. Uchee Pines is dedicated to helping people improve their health one choice at a time. With the rising rates of Diabetes, Obesity, Heart Disease, and Cancer in the United States, Uchee Pines Institute has for more than 70 years assisted people in restoring their health and wellness – mind, body, and spirit.
The God-fearing surgeon, when required to operate in critical cases, will call upon God for wisdom and help. And the Lord will honor His servant at such times, guiding the instrument he handles in the fear of God. At such times it is of the greatest importance that the physician be calm and able to speak words of faith and trust in the One who is our Creator and our King.
E.G. White - Kress Collection 165.2
Patient Education & Surgery Post Archives
- Surgery Archives
- Gallery Item
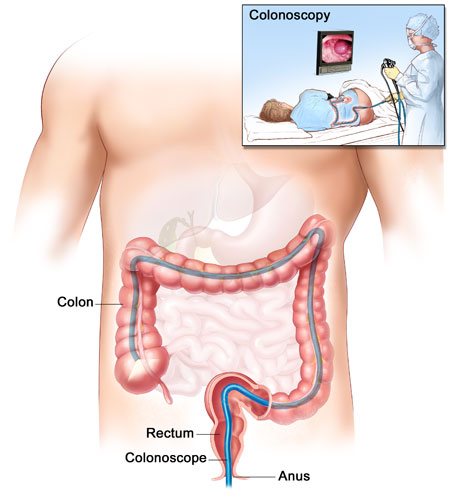
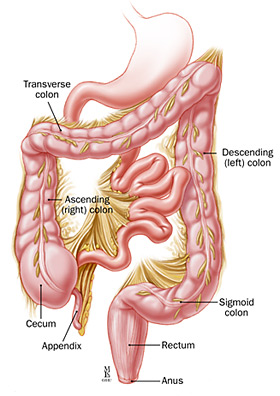
Colonoscopy
A whole lot of people avoid, put off, and just down right
refuse getting a colonoscopy. Especially if they don't have
any gastrointestinal issues, chronic belly pain, or change in
bowel habits. But let me tell you, better to "suffer" the
colonoscopy and know for sure and early than to wait and
find out late.
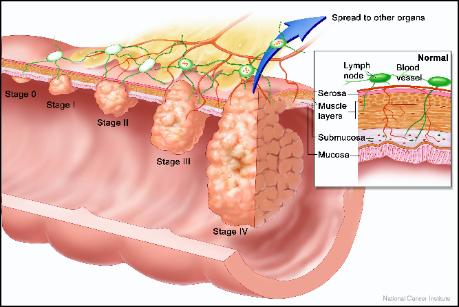
Colon Cancer
If you have cancer of the colon or rectum, your doctor will probably talk to you about
various treatment options. Surgery to remove the tumor is usually the main
treatment for colon and rectal cancer. Chemotherapy (treatment with drugs that kill
cancer cells) is often used when there is a risk that the colon or rectal cancer will
come back.
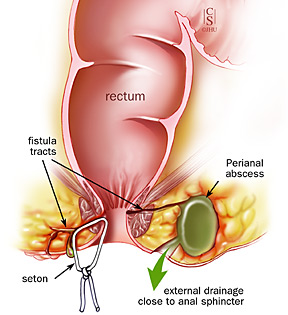
Perianal Abscess
When the tiny anal glands that open on the inside of the anus get blocked, the
bacteria that always live in the glands cause an infection. When pus forms, there is
an abscess (a pocket of pus). Treatment includes draining the abscess, usually
under local anesthesia in the doctor's office.
LIFESTYLE MEDICINE